COMMON CAUSES OF INFERTILITY
Infertility is tied to female factors in about 30% of the infertility cases, and male factors in about 35% of cases, the rest is related to unexplained causes. Here are some of the factors that cause infertility in women and men:
CAUSES OF INFERTILITY IN WOMEN
There are various reasons for infertility in women from physical problems such a blocked fallopian tubes to various hormonal imbalances.
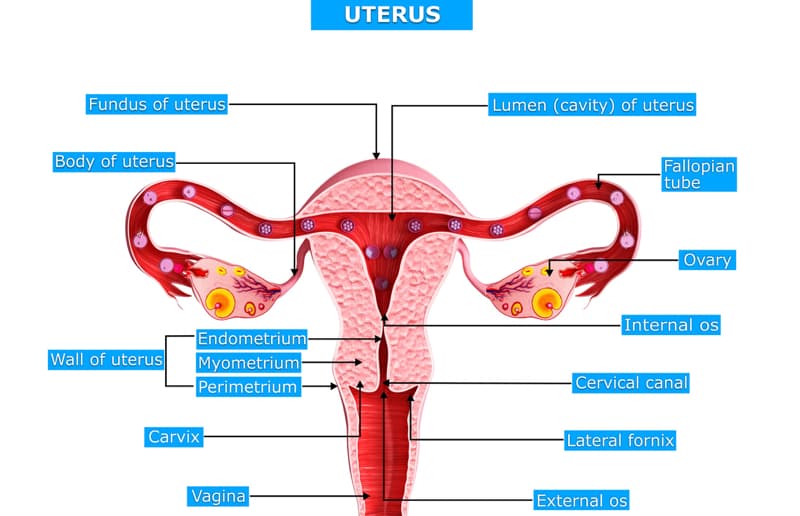
Female reproductive system front view
DAMAGED FALLOPIAN TUBES
A partial or complete blockage of the fallopian tubes caused by pelvic inflammatory disease, caused by STD’S such as chlamydia or gonorrhea; or scarring which can be caused by surgery, bacterial or viral infections, can interfere with conception by preventing the sperm from entering and reaching the egg.
PCOS
Formerly known as Steven- Leventhal syndrome, PCOS affects up to 10% of the women. In PCOS, the maturing follicles remain trapped in the ovary instead of being released at ovulation. Resistance to insulin and an overproduction of male hormone symptoms are largely responsible for the reproductive symptoms associated of infertility in women diagnosed with PCOS.
ENDOMETRIOSIS
Endometrium is a layer of tissue that lines the inside of the uterus. When this layer grows outside of the uterus, in areas such as the ovaries, outside the uterus, around the fallopian tubes, it can cause blockages, which can hinder conception or the development of a fertilized egg.
OVULATION PROBLEMS
A common cause of infertility in up to a quarter or more cases of infertility. Ovulatory problems due to an imbalance in LH, FSH and estrogen can interfere with ovulation thus preventing conception. Hypothyroid or underactive thyroid issues can also cause interference with the cycle regulation creating irregular periods and in turn cause fertility issues.
UTERUS AND CERVIX DISORDERS
An abnormally shaped cervix or having cervical mucus that is too thick or hostile to sperm can cause physical barriers that keep the sperm away from the egg. In some women, anti-sperm antibodies in the cervical mucus can overwhelm sperm, slow them down or even disable them until they are destroyed by white blood cells. Fibroids and polyps can also prevent a fertilized egg from attaching to the uterine wall.
The path to fertility and good health: If you have been diagnosed with any of the above, fear not! Naturopathic Medicine is great for balancing hormones, reducing fibroids and improving circulation to uterus, along with helping your overall health and immune function using natural therapies.
CAUSES OF INFERTILITY IN MAN
HORMONAL IMBALANCE
Male infertility can result if the body doesn’t produce enough testosterone or gonadotropins, which includes follicle-stimulating hormone (FSH) and luteinizing hormone (LH). Hormonal problems primarily can be traced back to either the primary glands (Hypothalamus, Thyroid, Pituitary) that produce the hormones or the glands that the hormones target (Prostate, Testes). If one of these glands malfunctions, this can cause problems in sperm production, or in the production of the milky nourishing fluids that make up semen.
Sperm
Sperm comprise a surprisingly small fraction of the semen itself (5%). Approximately 100 – 400 million sperm are present per ejaculate and they can survive up to 5 days in fertile cervical fluid. Low sperm counts and sperm abnormalities may be caused by hormonal problems, anatomical problems, immunological problems or even environmental factors.
The following are sperm-related abnormalities:
Azoospermia: No sperm in the semen. In some cases, sperm is produced in the testes, but there is an obstruction or malfunction that prevents the sperm from being ejaculated.
Oligozoospermia: Low sperm count.
Asthenozoospermia: Sperm with poor or low motility that impede their ability to swim well enough to reach the egg.
Teratozoospermia: Ill shaped sperm causing limited ability to fertilize the egg.Sperm can also be affected by the immune system. Possibly resulting from trauma or infection, the male body may produce antibodies that coat the sperm and cause the individual sperm to clump together.
BLOCKAGE
Any sort of obstruction in the sperm ducts, vas deferens, or urethra can prevent the sperm from being ejaculated. A common cause of infertility, blockages can be caused by infections (including sexually transmitted diseases), and can sometimes be repaired to restore fertility. A structural blockage may require surgery or some other procedure, while a blockage caused by infection may clear up with antibiotics and not need surgery. If the structural blockage cannot be repaired, then a testicular biopsy can be done to retrieve sperm.
Physical abnomalities include:
a) Hydrocele
A small bag of water might be present in the scrotum (the sac of skin surrounding the testicles). This rare condition can be treated surgically.
b) Retrograde ejaculation
Retrograde ejaculation occurs when semen is ejaculated into the bladder instead of exiting through the penis. Retrograde ejaculation is a malfunction in the valves that control the flow of urine versus semen through the urethra; this rare condition is sometimes the result of diabetes or the removal of the prostate gland.
If a man's system operates as it should, the valve between the bladder and the urethra constricts during ejaculation or conversely, the valve between the vas deferens and the urethra closes during urination.
c) Undescended testes (cryptorchidism)
The scrotum hangs outside the body because the temperature of the testes needs to be a few degrees cooler than body temperature for normal sperm production to occur. Fertility problems can develop if the testes do not descend into the scrotum within the first month or so after birth. Surgery can repair undescended testes, but permanent damage can sometimes result if the testes do not descend in childhood.
d) Varicocele
Varicose (enlarged) veins in the testicle cause varicocele. There is much debate about the relevance of a varicocele on fertility, but a prevailing theory is that the veins increase the temperature in the testicles. This heat weakens sperm and impedes sperm production. Varicocele can be surgically repaired.
e) Vasectomy
A common reason for the absence of sperm in the ejaculate is a previous vasectomy. Men can elect to have a surgical procedure done to reverse the vasectomy.
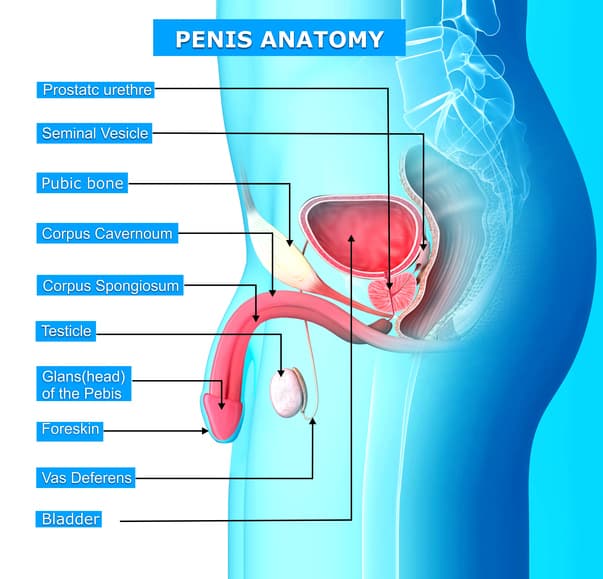
Male reproductive system side view
Related Articles
Acne
Acne is a common skin condition with a prevalence of 80% in female and 90% in male teenagers. It is caused by a disorder of the oil glands that result in clogged pores and outbreaks of lesions commonly known as pimples. Risk factors: poor diet, excessive sugar, trans fats and processed foods.
Candidiasis
Candida overgrowth in the gastrointestinal tract is now becoming recognized as a complex medical syndrome known as chronic candidiasis or the yeast syndrome. Symptoms include: Multiple food allergies, or allergic to all foods( pan allergic), alternating diarrhea with constipation.
Chronic Fatigue
Chronic Fatigue Syndrome (CFS) is described as a severe, debilitating fatigue, lasting at least six months (of new and definite onset), associated with at least four of the following symptoms: impaired memory or concentration, sore throat, muscle pains, joint pains, unrefreshing sleep and post-exertion malaise.
Irritable Bowel Syndrome
Irritable bowel syndrome (IBS) - a diagnosis of exclusion, this condition is often misdiagnosed. Severe food intolerances / allergies may exhibit symptoms that are similar to Irritable Bowel Syndrome such as pain, cramping, gassiness, sudden bouts of diarrhoea, and constipation.